Diabetes can be a difficult disease for a baby and parent. Physical, emotive, and psychological tolls occur on a daily basis for those living with diabetes. The rate of newly recognized patients has increased exponentially in recent times, inexplicably by doctors, still, awareness and education haven’t. It is crucial that in order to work at a cure for type 1 diabetes, an awareness of the disease, symptoms, therapy, management, complications, and avoidance must first be set up.
Diabetes exists in 2 forms-type 1 and kind 2 . Approximately 95% of individuals suffering from diabetes have kind 2, while only five per cent of Americans suffer from type one Though type 2, occasionally referred to as adult-onset diabetes, is more prevalent, type one, otherwise known as “juvenile” diabetic, is often considered the more serious from the two. Type 1 diabetes is most commonly diagnosed in children; however, it is possible to always be diagnosed in adulthood.
As soon as the body ingests food, typically the stomach begins to break down its contents into protein, extra fat, and carbohydrates. It is carbs that further break down into glucose, which the body purposes for energy. In a normal, healthful body, the pancreas produces a hormone called insulin, which helps the cells soak up and use the glucose. The actual insulin acts as a key toward the cell so that when it is launched, it opens the cellular allowing glucose to be assimilated. However, when insulin is usually absent, the cell can not open and absorb typically the glucose from the bloodstream.
A sort 1 diabetic’s pancreas will not function properly-it releases small to any of the junk, insulin, as it should. For that reason when glucose enters the actual bloodstream, it is forced to stay there because insulin is not really present to open the cellular for absorption. It is a step to understand that type 1 diabetes is “considered to be a good auto-immune disease because the insulin-producing beta cells in the pancreatic are attacked and ‘erroneously’ destroyed by the immune system in early stages in the disease process, leading to little to no insulin production within the pancreas”. Thus, a type one diabetic requires insulin treatment to maintain normal blood glucose quantities.
Diabetes is an auto-immune disorder that scientists believe is due to genes. Genes are “like instructions for how the human body should look and job… but just getting the gene history for diabetes isn’t normally enough. In most cases, something else should happen like getting a virus infection-for a person to get Type one particular Diabetes”. In other words, diabetes is simply not considered to be an infectious disorder, and it is not like a cold that could be caught by being inexperienced someone who suffers from the disease. However, doctors still cannot estimate who will develop the disease as well as who will not.
There are many traditional symptoms associated with type one diabetes that can develop possibly suddenly or gradually. The most typical symptom is frequent peeing, followed by increased thirst, weight reduction, fatigue, and increased hunger. If anyone experiences these symptoms, particularly if there is a family history of diabetes, it is important to seek medical attention instantly. Failure to treat these symptoms could bring other health problems such as “stomach pain, nausea, vomiting, problems with breathing, and even loss of consciousness. Medical professionals call this diabetic ketoacidosis or DKA”.
Currently, you cannot find any cure for type one particular diabetes; however, there are some therapies being explored. The three principal treatments being explored are generally Pancreas transplants, Islet cell phone transplantation, and Stem cell phone transplants. Pancreas transplants can be rare because of the risks connected with them. Upon transplantation, one could need a “lifetime of effective immune-suppressing drugs to prevent appendage rejection”. In addition to these immune-suppressing drugs, a “high probability of infection and organ injury” exists among those receiving an implant.
Islet cell transplantation “provides new insulin-producing cells from your donor pancreas”. Similar to a pancreatic transplant, islet cell hair transplant requires the use of immune-suppressing prescription drugs, which carry the same threats. The risk of the immune system destroying often the transplanted cells is also a possibility. Finally, stem cell place is another treatment being investigated. Stem cell transplantation will involve “shutting down the immune system and building it up again-[which] can be risky”. The entire group of these treatments are guaranteed, yet scientists are still functioning toward finding a more successful and also permanent treatment for diabetes.
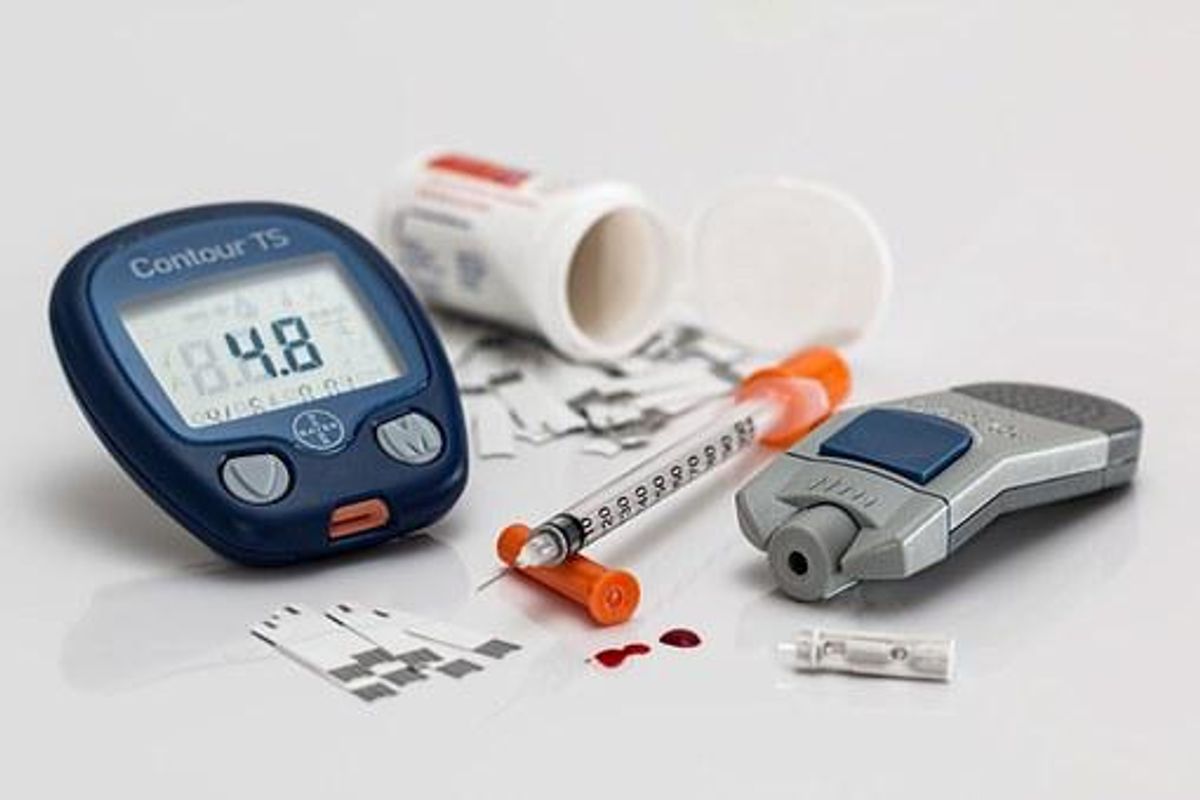
While there is no cure for diabetes, it is important to follow a rigid diabetes management plan so that you can live a healthy life. Typical blood glucose monitoring and insulin therapy are two critical forms of proper diabetes supervision. Fortunately, technological advancement as time passes has allowed blood glucose tracking to be very simple. Upon medical diagnosis, patients receive a blood glucose colocar to carry with them at all times regarding blood glucose testing.
This colocar allows a diabetic to be able to their blood glucose, or “blood sugar” level, at freedom in order to maintain better diabetic control. A meter simply requires a small drop of blood, and readings can be purchased in approximately five seconds. You should keep blood sugar levels between 50 and 120 as much as possible. In the event steady glucose levels are not looked after or diabetes management is definitely neglected over time, serious risks can result such as “seizures, loss of sight, kidney failure, heart attack, altération and strokes.
Insulin therapy constitutes another key to healthy diabetic management. Regular insulin amounts help control blood glucose degrees following meals and instantaneously. There are two main sorts of insulin: short-acting and long-acting. Short-acting insulin is managed during the day or following dishes. It is called short-acting as a result of a small amount of time needed for the insulin to take effect. This is especially crucial following meals because, because the body absorbs the blood sugar from food, blood glucose ranges rise quickly. Short-acting insulin combats the swift within glucose levels and helps maintain a gradual blood glucose reading.
The second form of insulin is a long-acting insulin. This is administered before going to rest at night because the insulin little by little acts upon glucose levels. As opposed to immediately having an effect on blood glucose levels, the long-acting insulin slowly applies by itself keeping glucose levels steady through the entire night. The amount or kind of insulin that a diabetic get varies from person to person-no one person is the same.
Like a diabetic becomes adjusted to their body and the disease, they are going to begin to assess their human body’s need for insulin. Some will need more insulin than other people, and this generally happens with time. As a diabetic patient is constantly on the life with the disease, their body will end up more and more dependent on synthetic, or even manufactured, insulin rather than it’s very own.
In addition to blood glucose monitoring as well as insulin therapy, a healthy diet, as well an active lifestyle, are steps to proper diabetes management. Coping with diabetes can mean making an important dietary adjustment for a freshly diagnosed patient. While excess fat, proteins, and carbohydrates could possibly have never been considered ahead of diagnosis, a type 1 diabetic’s diet revolves around them. Mindful planning and measuring involving food intake to insulin rate is strenuous and time consuming, yet essential.
It is important for the body to receive all of its essential nutrients while maintaining proper blood sugar levels. This requires careful working out of carbohydrate, or carbo, to insulin ratio. Every single diabetic has a standard rate of insulin per 1 carb. Fifteen grams associated with a carb is, for common purposes, considered one carbohydrate. Based on how many grams associated with carbs are in a meal, the actual ratio of insulin then can be calculated. It is difficult to imagine performing calculations like this for every dinner, but that is the reality associated with living with diabetes.
The final part of proper diabetes management is actually maintaining an active way of life. A proper lifestyle allows a person with diabetes to maintain better command over their diabetes. Currently being active helps lower sugar because “muscle contraction, enhanced blood flow and increased body temperature cause the body to be far more responsive or ‘sensitive’ for you to insulin during and shortly afterwards exercise. In addition, when muscle groups contract, they can take up carbs and glucose from the bloodstream independently associated with insulin”.
Since muscle compression can take up glucose through the bloodstream without insulin throughout exercise, being active is very encouraged when blood glucose amounts are elevated. This will assist bring high glucose levels right down to a more normal reading rapidly. Thus, a well-balanced diet plan and active lifestyle tend to be imperative to proper diabetic management.
Serious complications may evolve from poor administration of diabetes. Seizures, diabetic coma, ketoacidosis (ketones found in the bloodstream cause often the kidneys to shut down), losing vision, depression, amputation, in addition to premature death are all risks of diabetes. Lauren Stanford, at 13, felt often the frustrations of living with diabetes: “I wanted so bad for being like my other teenager friends who were free to stress about nothing more than boys and movies in addition to fun, ” she says. Lauren, like many teenagers, did start to neglect her diabetes as a way to feel “free” like different children her age.
But not only did she neglect to display her blood glucose levels, but she began skipping insulin doses as well. Lauren began to say, “On July 30th I collapsed and also was rushed to Kid’s Hospital in Boston just where I was put in the ICU. I possibly could have died. Diabetes practically got me”. Ignorance and also neglect of diabetes supervision can carry serious health threats as seen in Lauren’s history. It is important to realize that diabetes is just not a disease that will go away when ignored. Rather, serious difficulties can evolve from overlooked. Therefore, it is very important to handle Diabetic in a serious and dependable manner.
Type 1 diabetes is a serious disease that will carry serious consequences and also health risks from poor management. Therefore, the bruises, cracks, and tender skin by finger pricks and treatments are a necessary part of a lifetime for one living with diabetes.
Quite a few parents suffer from the guilt of hurting their child with regular sticks, but this is what maintains a child with diabetes living. Regular glucose monitoring, insulin therapy, a healthy diet, and a dynamic lifestyle are the most important ways of proper diabetes care. Quite a few children and adults suffer from type just one diabetes, but with the enhancements of technology, those affected by diabetes are able to live a nutritious and happy lifestyle right up until a cure is found.
Read also: